By: John Tate from Elite Chiropractic
Plantar fasciitis is a musculoskeletal condition that affects more than 1 million people per year. Simply put, it is inflammation of the plantar fascia – the interwoven tendons, ligaments, and connective tissue which stretches from the heel to the toes. This complex connective tissue acts like a shock absorber and a spring loading mechanism for the foot and ankle as we walk; it absorbs the impact of landing on the foot and elastically loads force to push off with that foot as we continue with our gait cycle. Plantar fasciitis is the condition where the fascia has been torn, bruised, or otherwise injured and has become inflamed. 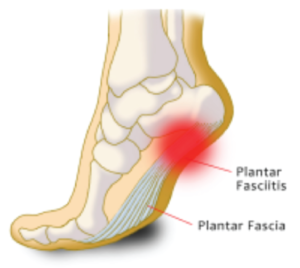
About 1 in 10 people will develop plantar fasciitis at some point in their lives. The most affected populations are young athletes and people who are obese. The pain can be debilitating. It can be caused by excessive ankle pronation (aka walking flat-footed, dropped arches, etc.), prolonged running, prolonged standing, and even obesity. Essentially, plantar fasciitis is caused by putting stress on the heel of the foot.
What are the symptoms of plantar fasciitis?
Plantar fasciitis has many symptoms, but the most commonly reported symptoms are pain on the bottom of the foot and/or heel, which is especially prevalent in the morning when you get up, or after exercising – not during exercise. It is also common to report having pain in the heel from standing after a long period of sitting. Heel pain that lasts for months is very indicative of plantar fasciitis as well. Plantar fasciitis pain usually gets better with use, so the pain decreases over the course of the day or the workout. Pain that lasts for months, and possibly years, is an important distinction of plantar fasciitis from other types of injuries.
How is plantar fasciitis diagnosed?
Plantar Fasciitis can be diagnosed by visiting a healthcare provider who will, after reviewing the patient’s medical history and their description of symptoms, perform a physical evaluation of the foot and ankle. Important red flags that they will look for include: putting pressure on the plantar fascia causes pain, placing the ankle and/or big toe into extension causes pain in the fascia near the heel, and whether the patient reported the positive signs of ‘pain which is worse in the morning, but gets better over the course of the day,’ and other previously mentioned symptoms. Usually, diagnostic imaging such as x-rays, ultrasound, or MRIs are not necessary to make the initial diagnosis of plantar fasciitis. You should ask your doctor about plantar fasciitis if you have long lasting heel pain which goes on for more than 2 weeks. If you follow recommended care guidelines for more than 6-8 weeks without results, you should check with your doctor again about other treatment options.
How is plantar fasciitis treated?
A healthcare provider can recommend several conservative treatments for plantar fasciitis which are beneficial to the majority of patients with this condition. These treatments are standard for taking care of other ligament damage injuries:
● Resting the injured tissue.
● Massaging the injured tissue.
● Putting ice on the affected area three to four times per day for 15 to 20 minutes. ● Wearing good supportive shoes with strong arch support.
● Do not wear sandals or flip flops, do not walk with bare feet.
Plantar fasciitis is usually treatable with these conservative measures – however, it usually requires a substantial change of daily habits to make sure that the condition does not return when normal activities resume. One should expect to make these conservative home-care recommendations part of their daily routine while they exhibit risk factors such as obesity, prolonged daily running or standing (especially on hard surfaces), and walking with excessive pronation; aka dropped arches, flat feet. You should talk to your doctor if, after you have tried these at-home treatments for more than 2 weeks, your symptoms have not improved. If you follow recommended care guidelines for more than 6-8 weeks without results, you should check with your doctor again about other treatment options, such as Shockwave Therapy, custom orthotics, custom splints for wearing at night, and if all else fails; injections and finally surgery.
Ways to reduce the risk of developing plantar fasciitis:

● Tape your arches, especially before you go on a long run, or are on your feet all day.
● Stretch your feet, ankles, calves, and Achilles tendons every day, especially if your work or exercise regimen puts you at a higher risk for injury.
● Ice your feet after a long day of work or running, to decrease the amount of inflammation build up in the tissue and to promote faster recovery.
● Change shoes regularly as a runner, always have a backup pair of shoes and always have good arch support.
Remember; if you have heel pain, you should see a healthcare professional about it. You may have plantar fasciitis, or a stress fracture, or another condition. If you don’t get your condition checked out and diagnosed, you won’t be able to know which therapies or at-home remedies you should be doing. If you are going to continue to run and work out with an injury, talk to someone like a physical therapist or a chiropractor about how to mitigate the long-term damage you could be doing to your body.
